This post presents background and key features on our new WikiJournal of Medicine article, “Working with Bipolar Disorder During the COVID-19 Pandemic: Both Crisis and Opportunity”.1 We are Emma Choplin and Caroline Vincent, two of the 13 authors of the paper, and we wrote this blog to inform the community about how those with Bipolar Disorder (BD) are at a heightened risk of catching COVID-19, require stigma-free and careful pharmaceutical treatment if they contract the virus and the hope that thoughtful technology-use can deliver cost-effective and tailored interventions to people in need. You can find the paper on PsyArXiv Preprints: https://psyarxiv.com/wg4bj/ and on WikiJournals:
In Chinese writing, the word for crisis combines the characters for “danger” and “opportunity”.
Need for the paper
The ongoing COVID-19 pandemic has to date infected more than 4.2 million people and led to more than 285 thousand deaths globally (projections of peak and incidence curve here). Businesses/work sectors are hurting, the stock market is still in turmoil, and the International Labour Organization projects that within the next three months there will be a decline in working hours equivalent to 230 million 40-hour a week employees not working.4
Higher Risk
People with Bipolar Disorder (BD) and related psychiatric conditions are a vulnerable population as a whole, because of potential environmental factors, often differing socioeconomic status, and health. This group can be at a higher risk of getting coronavirus due to environmental factors such as unstable or crowded living arrangements, reliance on public transit, and lack of social support. Those with BD are also more likely to smoke or use other substances, and to experience medical conditions such as obesity, diabetes mellitus, coronary heart disease, and obstructive pulmonary disease, which can make their cases of coronavirus more severe1. BD treatment plans can also complicate the treatment of COVID-19 due to complex drug interactions.
Resource: Drug Interaction Checker
Effects of COVID-19 people with Bipolar Disorder
“Stay-at-home” orders and quarantining are important tools to slow the spread of COVID-19, but they have high psychological and financial costs, especially for those with BD and related disorders.1 Their medical and mental health services have become much harder to access. Specifically, inpatient and outpatient care have been postponed or reduced; and many therapy services have stopped or moved online. For some, sheltering-in-place eliminates most of their social contact, access to news, and income while diminishing their quality of life. Beyond the public health and fiscal crisis, the COVID-19 outbreak intensifies stress, disrupts daily routines, and dysregulates sleep activity. Even in people without mental health challenges, disturbances in routine and sleep quality, limited stable space, and social isolation can cause negative psychological effects. For those with BD, the complex challenges of the pandemic can become the perfect breeding ground for unstabilized mood, interpersonal conflicts, self-destructive behaviors, and even suicide1.

Stigma
Social stigma rises when societies are under stress. Those with mental disorders, who can be considered contagious, or falsely “to blame,” are especially targeted. People with BD are more likely to experience stigma in their daily lives, and getting COVID-19 only increases the likelihood and level of stigmatization. When people with mental disorders develop a physical condition, medical concerns are likely to be discounted and undertreated, compromising the quality of care.
The added stigma may not only intensify sick BD patient’s sense of isolation but might invoke hostility from the healthcare workers towards them instead of the best medical support.
Silver lining
During this time of uncertainty, separation, and disarray, there are more obstacles for people with BD. Yet there are triumphs as well, when people proactively improve social connections, prioritize self-care, and utilize telehealth as an alternative to in-person treatment. The convenience and continuation of care can be what keeps clients/patients emotionally regulated and on-track. Mental health providers have answered the call for services by improving access to the best psychological and psychiatric interventions. Many have implemented telepsychology: treatment, clinical assessment, coaching, and safety planning delivered through telecommunication technologies, like telephones, videoconferencing, email, and self-help materials.
Resource: Telepsychology: Guidelines for Conducting Mental Health Services with Technology
Resource: Bipolar Disorder & Managing Stress during the COVID-19 Pandemic
Clinicians have been re-evaluating their safety plans with clients at-risk. Pre-existing services like phone and online support lines with trained counselors remain open to help those with suicidal thoughts escape distress, too. Professionals and community members have also worked to develop and spread more information on Reddit, social media, and Wikiversity, which are interactive platforms that share material quickly.
This infographic summarizes five ways of coping with COVID-19 and similar stressors.
Goals for the Bipolar & COVID-19 Paper
“Working with Bipolar Disorder During the COVID-19 Pandemic: Both Crisis and Opportunity” was written by a team drawing from many countries and many perspectives. We aimed to present careful considerations for delivering the best-tailored treatment for those with psychiatric disorders like BD, and how to operate by utilizing telecommunication in these unprecedented circumstances. This paper had 13 authors from China, Italy, Spain, the USA, and Canada, representing multiple cultures, many stages in careers, various educational backgrounds, and different areas of expertise, including a person with lived experience of BD. These different voices provide a well-rounded narrative with a trans-global element from multiple perspectives and angles.
What is WikiJournals, and why was it chosen?
Our goal is to spread reliable information as quickly, widely, and accessibly as possible to help people during these trying and uncharted times. That means avoiding exclusive journals, paywalls, and lengthy production processes. For these reasons, WikiJournal, an offshoot of Wikipedia, was chosen as the publication group for the paper. The WikiJournal User Group is an open-access, peer-reviewed academic group of journals that integrates content from branches of Wikipedia. It also allows the working paper to be widely shared even before peer review is finished. The edits are made live and tracked with a discussion function, making it conducive for large virtual collaboration. Like all Wikipedia sites, authors can keep the information up-to-date, continuing to improve the paper at each stage. The citable indexed publication has a greater reach than traditional scholarly publications, too. These factors made WikiJournals the best choice, since time was of the essence, and COVID-19 news, resources, and recommendations are always changing and growing.
About the Authors
Emma Grace Choplin, B.S.
In 2019, I received my B.S. in Psychology, minoring in Neuroscience and Religious Studies at the University of North Carolina-Chapel Hill where I researched Evidenced-Based Assessment and Dissemination & Implementation Science in Eric Youngstrom’s Lab. As a Past-President of Helping Give Away Psychological Science, I help bridge the gap between clinicians, academics, and the public to increase open-access to psychological science. I’m Dr. Elizabeth Losin’s Social and Cultural Neuroscience Lab’s Research Coordinator/Lab Manager at the University of Miami researching health disparities, doctor-patient relationships, and biased analgesic prescribing/decision-making. This Fall I’m applying to Clinical Psychology Ph.D. programs.
Caroline Vincent
I am an undergraduate at the University of North Carolina at Chapel Hill majoring in psychology and minoring in computer science and neuroscience. I work as a research assistant at UNC. I am the President of the UNC chapter of HGAPS. HGAPS helped work on the original article and add resources. The organization is dedicated to helping the best information about psychological science reach the people who would benefit.
HGAPS:
Instagram: @hgapsoranization
Twitter: @_hgaps
References and Resources
- Youngstrom E, Stefana A, Chen J, Michael K, Van Meter A, Maxwell V, Michalak EE, Choplin EG, Smith LT, Vincent C, Loeb A, Vieta E. Working with Bipolar Disorder During the COVID-19 Pandemic: Both Crisis and Opportunity. WikiJournal Preprints. Published online 2020.
- COVID-19 Map – Johns Hopkins Coronavirus Resource Center. Accessed May 11, 2020.
- IHME | COVID-19 Projections. Institute for Health Metrics and Evaluation. Accessed May 11, 2020.
- COVID-19 and the world of work (COVID-19 and the world of work). Accessed May 11, 2020.
- Types of Psychiatric Disorders. Verywell Mind. Accessed May 11, 2020.
- Homelessness and mental health. In: Wikipedia. ; 2020. Accessed May 11, 2020.
- The economic, geopolitical and health impacts of COVID-19. World Economic Forum. Accessed May 11, 2020.
- Mental Health Conditions Similar but Distinct from Bipolar Disorder. Accessed May 11, 2020.
- Stigma and discrimination. Mental Health Foundation. Published August 7, 2015. Accessed May 12, 2020.
- Bipolar Disorder & Managing Stress during the COVID-19 Pandemic | Psychiatry Michigan Medicine. Psychiatry. Published April 3, 2020. Accessed May 12, 2020.
For further references, check the WikiJournal article!
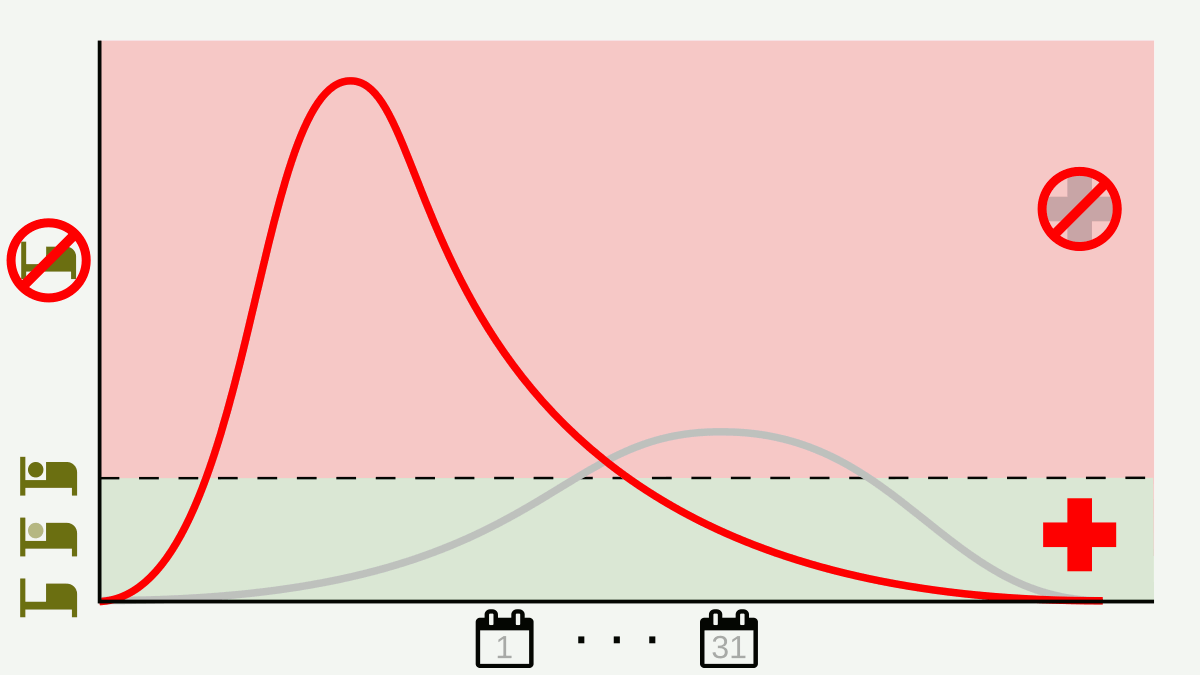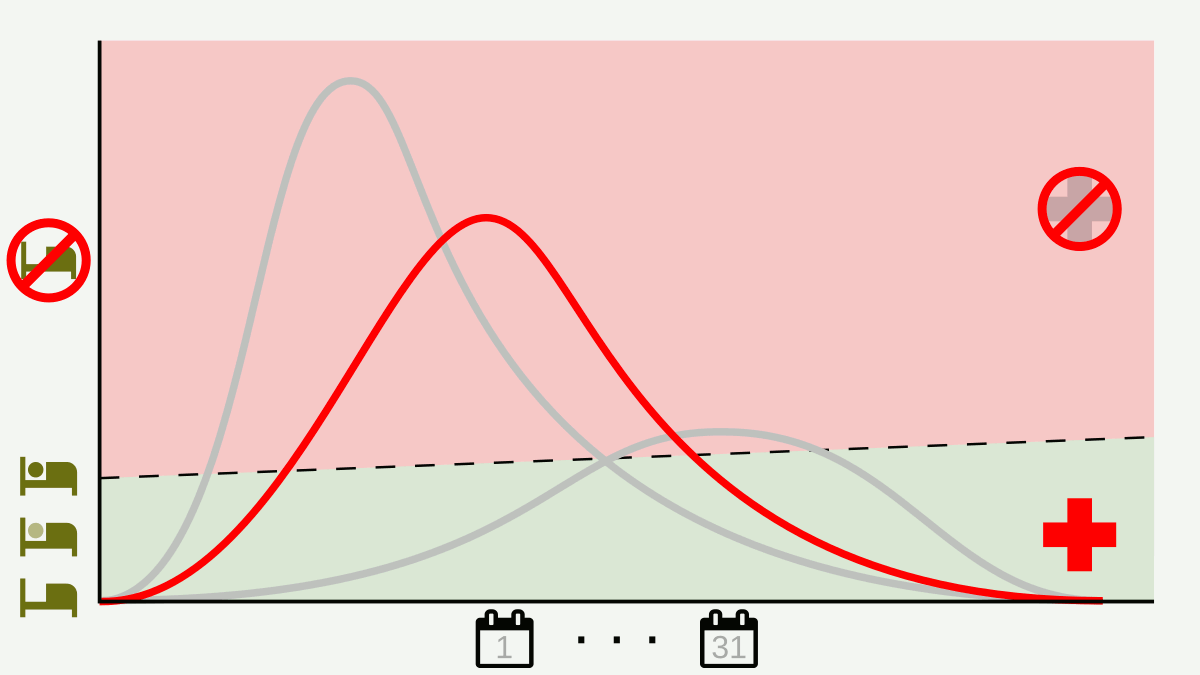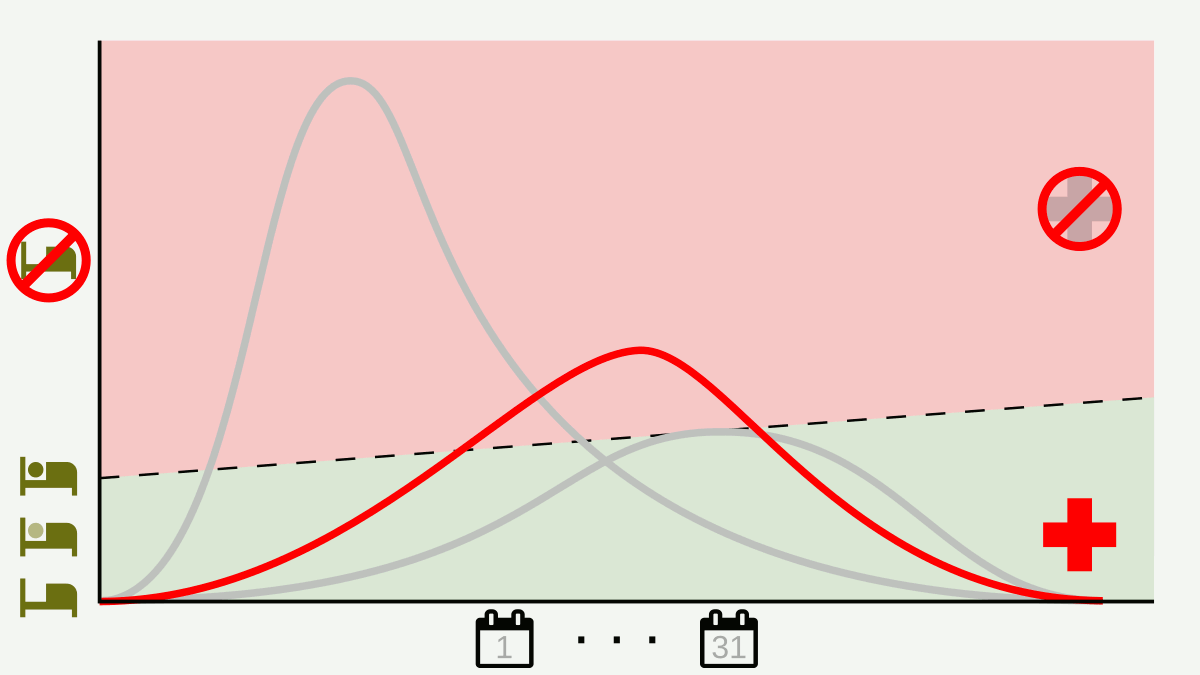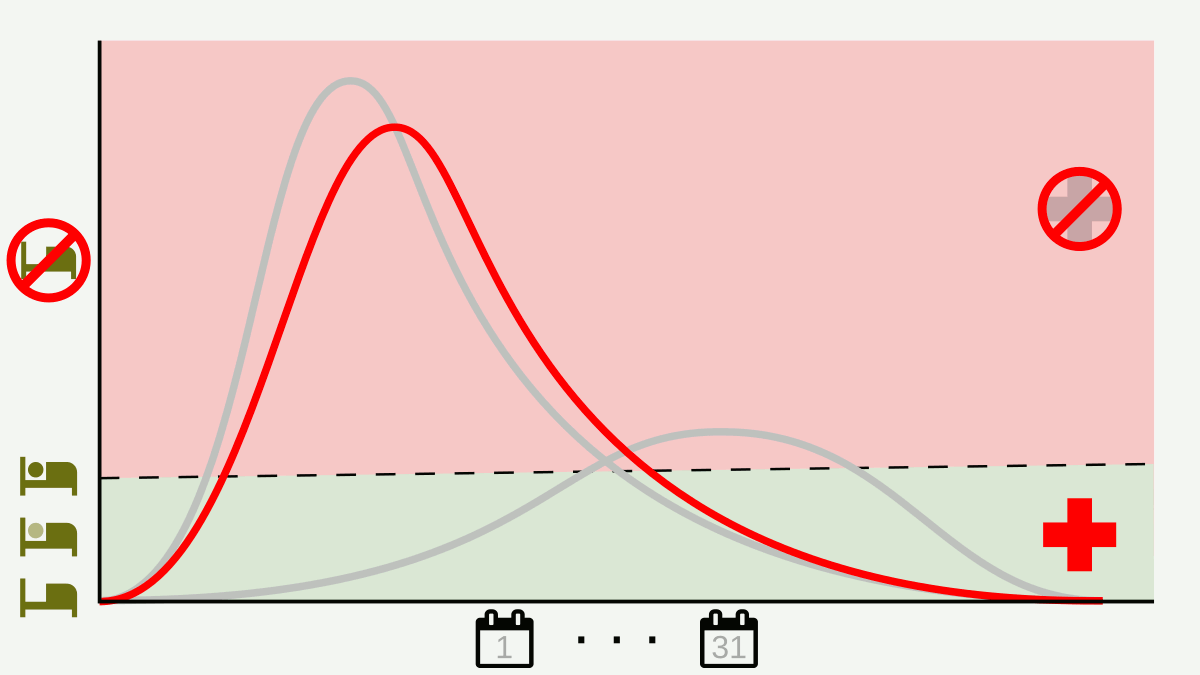




Excellent presentation with professional research while the subject matter was covered with respect to detail.
Wonderful article. I’m sure it will be beneficial to so many people with BD especially in this trying time of isolation. Very insightful!