Research on new treatments for depression and bipolar disorder typically test their effectiveness in a few specific ways. Usually, clinical trials investigating new pharmacological or psychological interventions are considered successful if they can:
- reduce symptoms
- delay the onset of new episodes
- lower the number of hospitalizations, and
- lower other treatment costs
But according to people who live with mood disorders, these criteria don’t capture all of what it means to live well. This is why involving people with lived experience is so important. By asking them what it means to live well, researchers and clinicians can make sure we’re measuring what matters.
The Supporting Wellness Project
So what aspects of wellness do people with mood disorders consider most important? The Depression and Bipolar Support Alliance (DBSA) created the “Supporting Wellness” project to explore this question.[1] To analyse and report on the project’s findings, the DBSA partnered with the National Network of Depression Centers (NNDC), as well as two CREST.BD researchers, Dr. Emma Morton and Dr. Erin Michalak. The project used community input to develop a survey asking people to describe their experiences living with depression or bipolar disorder, their perspectives of treatment, and their wellness priorities.
Over 6,000 people with depression or bipolar disorder completed the survey. Participants reported that, when they seek healthcare treatment, their goal is to function as well as possible. However, they often found their treatment as only focused on mood symptoms. The four priorities participants rated the highest were:
- the ability to act independently
- purpose in life
- getting through the day, and
- experiencing feelings of contentment.
A series of follow-up focus groups were conducted to deepen understanding of the survey results.
How to Use These Findings
These findings highlight how important it is to ask people with lived experience of mood disorders what they need to consider themselves ‘well’. While reducing symptoms is an important goal, for people with mood disorders, it’s not the whole picture. They also value functioning, quality of life, and a sense of overall wellbeing.
DBSA intends to use these findings to guide future research. Specifically, they plan to use this knowledge to inform what kinds of outcomes are important to measure in clinical trials and as part of measurement-based care for mood disorders.
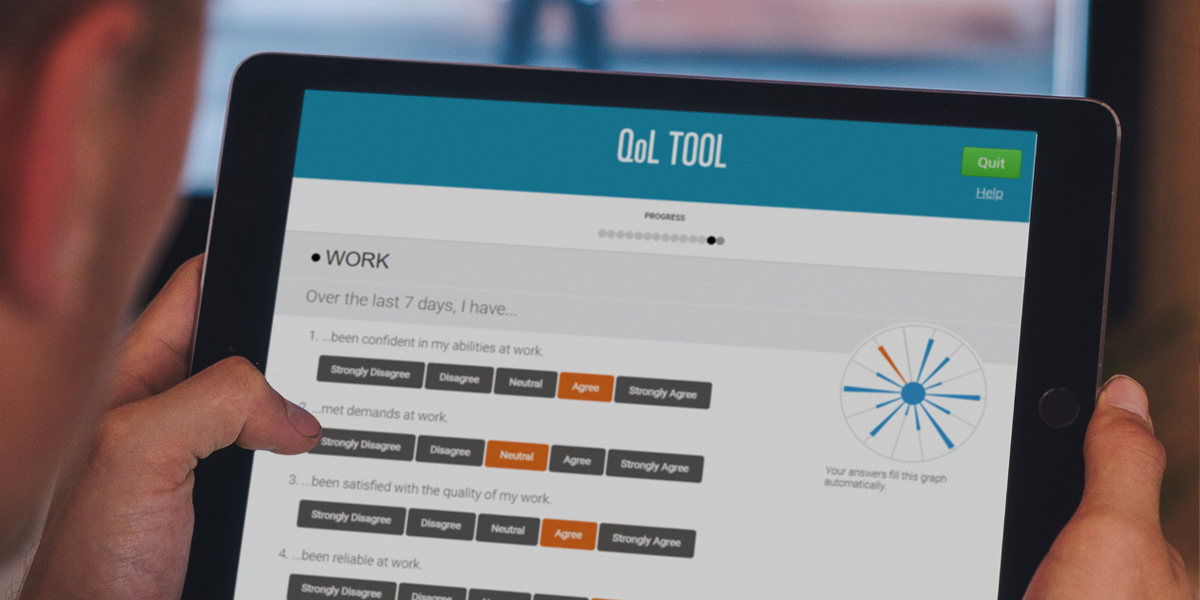
One way to do this is using the CREST.BD Quality of Life in Bipolar Disorder questionnaire.[2, 3] The QoL.BD provides an easy way for people to see what areas of life they are flourishing in, and those that may need some attention. To learn more about how we developed the questionnaire with community input, and how it might help you manage your health and wellbeing, check out the online Quality of Life Tool here.[4]
References
- Morton, E., Foxworth, P., Dardess, P., Altimus, C., DePaulo, J. R., Talluri, S. S., Michalak, E. E., Rinvelt, P. D., Corrigan, P. W., & Turvey, C. (2022). “Supporting Wellness”: A depression and bipolar support alliance mixed-methods investigation of lived experience perspectives and priorities for mood disorder treatment. Journal of Affective Disorders, 299, 575–584.
- Michalak, E. E., Murray, G., & CREST.BD. (2010). Development of the QoL.BD: A disorder-specific scale to assess quality of life in bipolar disorder: Development of the QoL.BD. Bipolar Disorders, 12(7), 727–740.
-
Morton, E., Murray, G., Yatham, L. N., Lam, R. W., & Michalak, E. E. (2021). The Quality of Life in Bipolar Disorder (QoL.BD) questionnaire a decade on – A systematic review of the measurement of condition-specific aspects of quality of life in bipolar-disorder. Journal of Affective Disorders, 278, 33–45.
- Morton, E., Hou, S., Fogarty, O., Murray, G., Barnes, S., Depp, C., Michalak, E.E., CREST.BD. (2020). Web-based adaptation of the Quality of Life in Bipolar Disorder (QoL.BD) questionnaire: A psychometric evaluation study. Journal of Medical Internet Research Mental Health 7(4):e17497.




Leave a Reply