It’s no surprise that people with bipolar disorder are increasingly using apps to manage their mental health1. Apps offer a lot of benefits – they are portable and affordable, which makes them a useful tool for people who might otherwise not be able to access in-person mental health care (due to cost, location, or stigma). In addition, apps can provide in-the-moment support when people really need it – this can help them better integrate self-management strategies in their everyday lives, or get help in-between appointments. However, unfortunately, not all publicly available apps meet appropriate standards in terms of their scientific backing, privacy protections, and safety2. Research teams (including CREST.BD) are looking to develop evidence-based, engaging digital tools, but this process takes time. In the meantime, clinicians may be able to play an important role in helping people identify and integrate safe and effective apps into their self-management plans.
“Unfortunately, not all publicly available apps meet appropriate standards in terms of their scientific backing, privacy protections, and safety.”
To understand the role clinicians might be able to play, it’s important to know if clinicians are currently recommending apps to people with bipolar disorder–and if not, why. This information may help us develop training resources for healthcare providers, and make effective plans for including apps in real-world clinical practice. In 2020, the CREST.BD team conducted a large-scale international web-based survey about how apps might be used to support people with bipolar disorder. We recently published a peer-reviewed paper describing how clinicians perceive and discuss apps when working with people with bipolar disorder.
Eighty healthcare providers from around the world completed the survey, and about half of these respondents said that they discussed apps when working with patients with bipolar disorder. However, clinicians expressed a low level of knowledge and confidence in recommending apps, and of clinicians who did not recommend apps, lack of knowledge about safe/effective apps was described as a major barrier.
It’s understandably difficult for clinicians to keep up to date with the rapidly evolving digital health landscape – there are over 10,000 mental health apps listed in the Google Play and Apple stores3, and new apps are being released all the time. Researchers can help time-pressed clinicians evaluate the safety and efficacy of publicly available apps. For example, the Division of Digital Psychiatry has an online database of crowdsourced app ratings completed by trained volunteers (https://apps.digitalpsych.org/). Providing education on evaluating and using digital health tools in clinical training is also necessary to help support the next generation of clinicians (see an earlier CREST.BD blog reflecting on digital health training by a med student here).
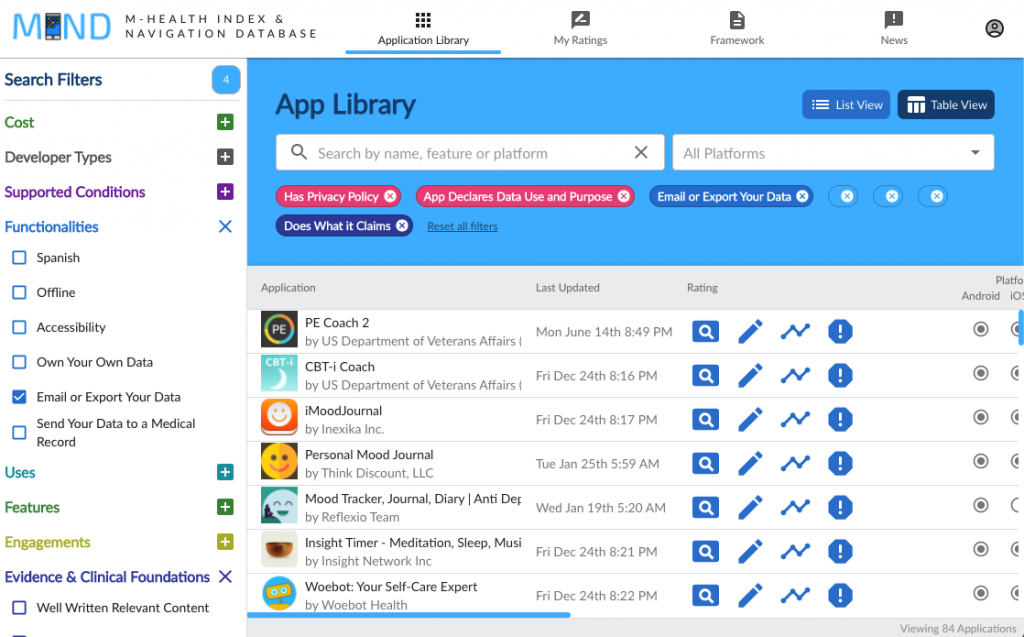
A screenshot of the app library in the mHealth Index & Navigation Database
Optimistically, more clinicians in our sample reported discussing apps compared to similar surveys in the recent past4. It’s possible that clinicians in our survey might have a higher level of confidence and knowledge about apps than in earlier years because of COVID-19 – physical distancing measures were implemented in early 2020 in most countries, meaning that healthcare providers have been learning a lot about ways to support their clients with digital tools. Although we hope that a brighter future is on the horizon in terms of pandemic-related restrictions, perhaps there are important lessons about digital health that healthcare providers can take with them into their clinical practice in future.
References
1. Diego Hidalgo-Mazzei, Viktoriya L. Nikolova, Simon Kitchen & Allan H. Young (2019) Internet-connected devices ownership, use and interests in bipolar disorder: from desktop to mobile mental health, Digital Psychiatry, 2:1, 1-7, DOI: 10.1080/2575517X.2019.1616476
2. Lagan, S., Ramakrishnan, A., Lamont, E. et al. Digital health developments and drawbacks: a review and analysis of top-returned apps for bipolar disorder. Int J Bipolar Disord 8, 39 (2020). https://doi.org/10.1186/s40345-020-00202-4
3. Torous, J., Andersson, G., Bertagnoli, A., Christensen, H., Cuijpers, P., Firth, J., Haim, A., Hsin, H., Hollis, C., Lewis, S., Mohr, D.C., Pratap, A., Roux, S., Sherrill, J. and Arean, P.A. (2019), Towards a consensus around standards for smartphone apps and digital mental health. World Psychiatry, 18: 97-98. https://doi.org/10.1002/wps.20592
4. Schueller, S.M., Washburn, J.J., Price, M., 2016. Exploring mental health providers’ interest in using web and mobile-based tools in their practices. Internet Interv. 4(2), 145-151.




Leave a Reply